Emergency Dentistry
Root Canal Recovery, Visits, and What Actually Happens in the Chair
A root canal typically takes one to two appointments and most people feel back to normal within a few days. But recovery isn't one-size-fits-all — a tooth with an active infection heals differently than one treated early. Here's what I want my Riverside patients to know before they sit down. If you're dealing with a dental emergency, understanding what to expect can make all the difference.
The Two Recovery Timelines Nobody Talks About
Most articles tell you "two to three days" for recovery. For Riverside-area patients, that's true for a straightforward case. But I find it more useful to split this into two distinct situations, because the experience can be very different.
Standard pulpectomy (no active abscess): Your tooth was treated before the infection became severe. After the procedure, expect mild tenderness and some jaw soreness for two to four days. Over-the-counter ibuprofen or acetaminophen handles this well. Cleveland Clinic confirms that most people recover in under a week, with lingering sensitivity that fades on its own.
Hot tooth / abscessed tooth: This is a different story. When there's a throbbing, active infection at the root tip, your immune system is already in overdrive. After we clean the canals, that immune response doesn't just switch off — it can actually intensify in the first 24 to 48 hours as your body reacts to the disruption of infected tissue. Some patients experience a "flare-up," meaning pain temporarily increases before it improves. In these cases, I often place a medicated dressing — typically calcium hydroxide — inside the canal and schedule a second visit to seal the tooth only after confirming the infection has cleared. This isn't a complication. It's deliberate, careful treatment.
There's also a musculoskeletal recovery factor that almost no one mentions. Keeping your mouth open for 60 to 90 minutes with a rubber dam and bite block puts real strain on the masseter and temporal muscles. Many patients report what feels like ear pain or jaw tightness afterward and worry the procedure failed. Usually, it's muscle fatigue or mild TMJ strain from the extended opening. Moist heat applied to the jaw joint helps more than ice for this type of discomfort. If your temporary filling feels even slightly high, call us — a bite that's off by even a millimeter creates muscle tension that compounds this soreness significantly.
What Actually Happens During the Procedure
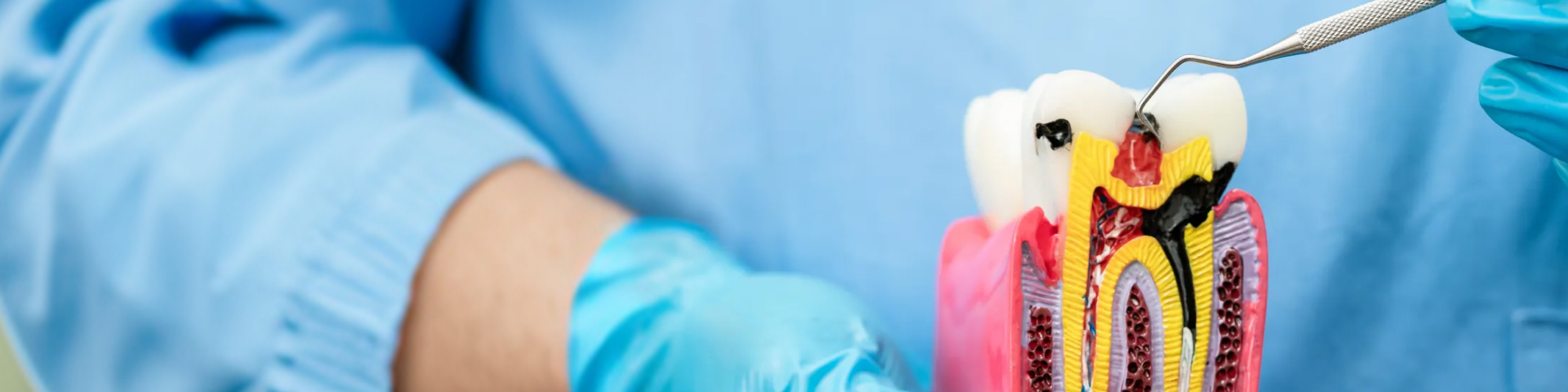
The goal is straightforward: remove infected or inflamed pulp, clean the canal space thoroughly, and seal it so bacteria can't re-enter. According to the American Association of Endodontists, this process eliminates bacteria from the infected root canal, prevents reinfection, and preserves the natural tooth.
Here's the sequence:
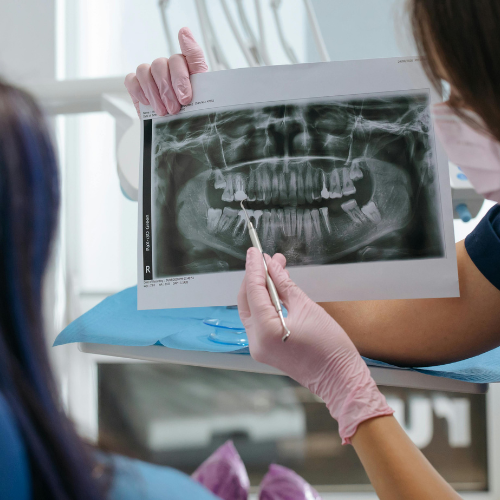
- X-rays and examination — I evaluate the extent of infection and canal anatomy before touching the tooth.
- Local anesthesia — The area is fully numbed. You may feel pressure during cleaning, but you shouldn't feel pain.
- Dental dam placement — A rubber sheet isolates the tooth, keeping it clean and free of saliva bacteria.
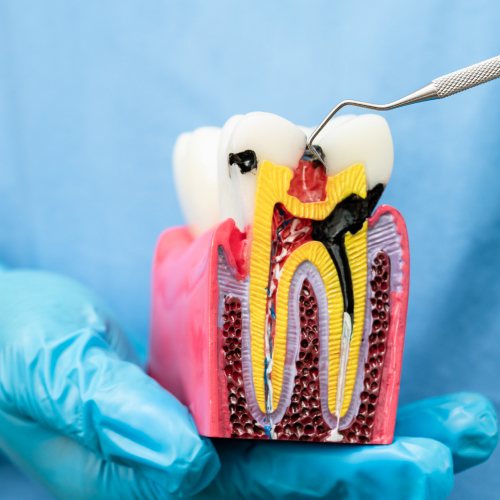
- Access opening — A small hole is made through the crown to reach the pulp chamber.
- Pulp removal and canal shaping — Small instruments remove the damaged tissue and shape the canals for filling.
- Irrigation — The canals are flushed repeatedly to remove debris and reduce bacterial load.
- Filling and sealing — Canals are filled with gutta-percha, a biocompatible rubber-like material, then sealed.
- Temporary or permanent filling — Depending on whether a tooth crown is planned, a temporary filling protects the tooth until the next visit.
Harvard Health notes that contrary to popular belief, the tooth roots remain intact — only the pulp tissue is removed. The tooth continues to be nourished by surrounding tissues.
The Temporary Filling Phase: A Window Most Patients Underestimate
If your root canal is completed over two visits, you'll leave the first appointment with a temporary filling. This phase — typically one to three weeks — carries specific risks that are worth understanding.
Temporary filling material is intentionally softer than a permanent restoration. It seals adequately under normal conditions, but it's porous compared to a permanent crown. If it chips, cracks, or wears down, bacteria from saliva can seep back into the cleaned canal space — a process called microleakage. This is why I tell patients to avoid chewing hard or sticky foods on that side entirely during this window.
Your tooth is also more prone to vertical fracture during this period than it was before treatment. Once the pulp is removed, the tooth loses internal moisture and becomes more brittle. Without the structural support of a permanent crown, a hard bite on the wrong food can split the tooth — potentially beyond repair. In some cases where the tooth cannot be saved, a tooth extraction may ultimately be necessary.
If your temporary filling feels "sandy" or loose, or if you notice it's partially come out, contact us promptly. The AAE's post-treatment guidelines are clear: getting the permanent crown placed quickly after your endodontic work is completed is one of the most important factors in long-term success.
One Visit or Two? How We Decide
Research published in PMC comparing single-visit versus multiple-visit root canal treatment found no significant difference in long-term radiological outcomes between the two approaches. So the number of visits isn't about one method being superior — it's about what your specific tooth requires.
Single-visit treatment works well when the infection is contained, the canal anatomy is straightforward, and there's no active abscess requiring a medicated dressing period. It reduces your total chair time, eliminates the temporary filling vulnerability window, and gets you to a permanent restoration faster.
Multiple visits make more clinical sense when there's a draining abscess, complex canal anatomy, or when I want to confirm infection has resolved before sealing. Untreated gum disease and gingivitis can also complicate the healing process and may need to be addressed alongside endodontic treatment. According to Healthline, a root canal can take anywhere from 90 minutes to three hours across one or more appointments depending on the tooth and severity of infection.
Molars, with their multiple roots and curved canals, almost always take longer than front teeth. I discuss this with every patient before we begin so there are no surprises about scheduling.
Ready to Talk Through Your Options in Riverside?
If you're experiencing tooth pain, sensitivity, or you've been told you need an endodontic root canal, I want you to feel informed — not anxious — before your appointment. At Dental Specialists of Riverside, we treat patients from across the Inland Empire, including Riverside and Corona, and we take the time to walk through your specific situation before any treatment begins. Reach out to schedule a cleaning and exam or consultation and get the clarity you deserve.
Medical disclaimer: This article is for informational purposes only and does not constitute medical or dental advice. Always consult a qualified dental professional for diagnosis and treatment recommendations specific to your situation.












..png)


..png)